Commonwealth Radiology Associates
Vascular & Interventional Radiology
Interventional Radiology (IR) is one of the most exciting advancements of modern medicine.
Many conditions once treated surgically can now be managed less invasively by interventional radiologists. Using high tech imaging, interventional radiologists can diagnose and treat a wide variety of medical problems, often on an outpatient basis, through a tiny incision, with less risk, less discomfort, and less recovery time compared to surgery.
Below are listed some of the conditions we can help manage.
Peripheral Arterial Disease
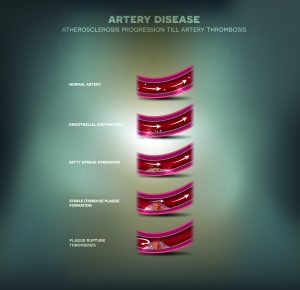
Artery disease, Atherosclerosis progression, narrowed artery and at the end blood clot block artery.
An estimated 10 million Americans have peripheral arterial disease (PAD) also known as peripheral vascular disease. It is a condition in which the arteries that carry blood to the legs and arms become narrowed or clogged by plaque, reducing normal blood flow and causing pain with exertion and possibly non-healing wounds. PAD is most commonly seen in patients over age 50, and those who smoke, have diabetes, high blood pressure or high cholesterol.
Treatments include:
- Angioplasty
- Stenting
- Atherectomy
- Thrombolysis
Venous Disease
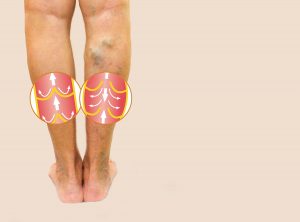 Venous disease can affect the deep or superficial veins in various ways.
Venous disease can affect the deep or superficial veins in various ways.
Varicose veins are bulging leg veins caused by malfunctioning valves. Normally valves inside the vein act as one way doors, keeping blood returning to the heart from the feet from refluxing, or flowing backwards, down the leg with gravity. When the valves in superficial veins malfunction, blood begins to pool in the leg veins and they enlarge. For many patients, varicose and spider veins are a cosmetic concern but for some patients the problem can progress to more serious conditions including leg fatigue, pain, swelling, brown discoloration, skin ulcers and blood clots.
Treatments include:
- Endovenous Radiofrequency Ablation
- Microphlebectomy
- Compression stockings
- Sclerotherapy
Locations:
- Vascular Specialists of the North Shore, Beverly, MA
- The Vein Center, Saints Medical Center, Lowell, MA
Deep vein thrombosis (DVT) is a serious potentially life-threatening condition where a blood clot forms in the major deep veins, usually of the leg or pelvis, and blocks blood return causing significant pain or swelling. A patient with DVT may be at risk of a pulmonary embolism (PE) when part of the clot breaks off and travels to the lungs. Risk factors include obesity, prolonged immobilization, pregnancy or certain health conditions. DVT diagnosis is made with ultrasound. (this prior section is NOT expanded)
Treatments include:
- DVT thrombolysis
- IVC filter placement
Cancer
Interventional Radiology works as part of a multidisciplinary treatment team to aid in diagnosing and managing certain types of cancer. Our role covers a wide range of procedures from image-guided biopsy, to port-a-catheter placement, to treatment itself. We offer transarterial chemoembolization (TACE) and Y-90 embolization for patients with nonresectable primary liver tumors and certain kinds of liver metastases to improve survival rates and symptom control. We also offer microwave and cryoablation which use thermal energy to treat inoperable tumors of the liver, lung, kidneys, adrenal glands, bone, and occasionally soft tissues.
Treatments include:
- Chemoembolization
- Y-90 embolization
- Microwave ablation
- Cryoablation
Pain Management
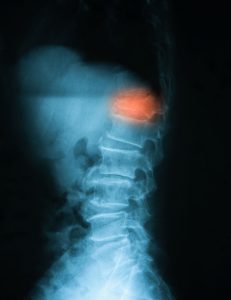 Interventional Radiology performs a diverse set of procedures to treat pain of various causes.
Interventional Radiology performs a diverse set of procedures to treat pain of various causes.
Treatments include:
- Kyphoplasty for compression fractures
- Sacroplasty for sacral insufficiency fractures
- Steroid joint injection
- Celiac plexus nerve block
Liver disease
The liver is essential for metabolizing nutrients and detoxifying contaminants gathered from the gastrointestinal tract and other organs by specialized blood vessels called the portal venous system. Cirrhosis of the liver is due to progressive scarring of the liver caused by a variety of conditions including chronic hepatitis, alcohol abuse, or biliary disease. As cirrhosis worsens it reduces the liver’s ability to produce proteins and remove toxins. Eventually, it obstructs the blood flow out from the intestines and spleen and can lead to gastrointestinal (GI) bleeding, ascites, and pleural effusions. Symptoms of cirrhosis may not be detected until severe irreversible damage to the liver has already been done. IR can assist in the diagnosis and staging of liver disease via biopsy and can address GI bleeding due to portal hypertension with Transjugular Intrahepatic Portosystemic Shunt (TIPS).
Treatments include:
- Percutaneous or transjugular liver biopsy
- TIPS
- Balloon-occluded Retrograde Transvenous Obliteration (BRTO)
Kidney failure
 The kidneys filter blood to remove excess fluid and toxins by producing urine. When the kidneys do not work properly, fluid and contaminants build up and can have severe potentially life-threatening effects. Acute kidney failure occurs over a matter of hours to days and can be caused by a variety of conditions such as an obstruction of urine outflow, loss of blood supply to the kidney, infection, etc. Chronic kidney disease (CKD) is a slow decline in kidney function. Risk factors include diabetes, hypertension, heart disease, smoking, obesity, high cholesterol, and age over 65 yrs.
The kidneys filter blood to remove excess fluid and toxins by producing urine. When the kidneys do not work properly, fluid and contaminants build up and can have severe potentially life-threatening effects. Acute kidney failure occurs over a matter of hours to days and can be caused by a variety of conditions such as an obstruction of urine outflow, loss of blood supply to the kidney, infection, etc. Chronic kidney disease (CKD) is a slow decline in kidney function. Risk factors include diabetes, hypertension, heart disease, smoking, obesity, high cholesterol, and age over 65 yrs.
Treatments include:
- Percutaneous nephrostomy tube
- Ureteral stent
- Hemodialysis vascular access
- Arteriovenous fistula maintenance
Enteric Access
Using x-ray guidance we place and exchange gastrostomy and gastrojejunostomy tubes for patients who are unable to tolerate eating by mouth.
Women’s Health
Pelvic congestion syndrome is an often-unrecognized cause of chronic pelvic pain caused by abnormally functioning enlarged veins in the pelvis. Patients can have pain and heaviness in their pelvis which worsens with prolonged standing. It can be suspected by abnormal pelvic veins on ultrasound and further evaluated by MRI.
Uterine fibroids are common noncancerous growths that develop in the wall of the uterus and can cause significant discomfort, heavy menstrual bleeding, pain during intercourse, bladder pressure/frequent urination, and constipation. Surgical options include hysterectomy and myomectomy but fortunately, most woman are candidates for a minimally invasive non-surgical option.
Treatments include:
- Pelvic venogram and embolization
- Uterine artery embolization (UAE)
Men’s Health
 A varicocele is an enlargement of veins in the scrotum surrounding the testicle. Veins normally contain one-way valves that allow blood to flow from the testicles and scrotum to the heart against gravity. When these valves malfunction, the blood pools in the scrotal veins. The increased pressure and temperature can cause infertility.
A varicocele is an enlargement of veins in the scrotum surrounding the testicle. Veins normally contain one-way valves that allow blood to flow from the testicles and scrotum to the heart against gravity. When these valves malfunction, the blood pools in the scrotal veins. The increased pressure and temperature can cause infertility.
Benign prostatic hyperplasia (BPH) is a common condition affecting nearly half of men in their 50s and approximately 90 percent in their 70s and 80s. It is noncancerous enlargement of the prostate, a gland next to the bladder, which can cause urinary symptoms such as incomplete emptying of the bladder, urinary frequency, and nighttime urination, all significantly impacting quality of life.
Treatments include:
- Varicocele embolization
- Prostatic Artery Embolization (PAE)
Cosmetic
Our Board Certified Physicians provide treatment for fine lines and wrinkles using Botox and Juvederm. We also provide state-of-art laser hair removal.
Locations:
- Look Your Best North Shore Medical Spa, Beverly, MA
Peripheral Arterial Disease
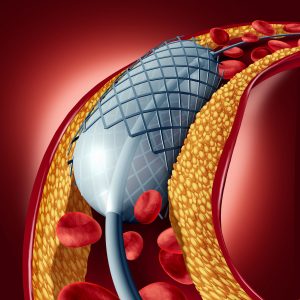 Angioplasty
Angioplasty
During angioplasty, using x-ray guidance, a catheter or thin hollow tube is passed through a blood vessel to the area of blockage. A balloon is inflated and breaks open the narrowing. Depending on the severity and location of the blockage, an interventionalist might also shave off part of the blockage (atherectomy) or place a stent (a tiny metal brace which keeps the artery open).
Thrombolysis
Thrombolysis treats acutely blocked arteries. This is usually an emergency treatment performed when the clot happens so quickly that the body has not had time to grow new blood vessels to bypass the blockage. A thin tube is inserted through a tiny incision into a blood vessel and advanced into bthelocked artery. Medication is delivered through the tube into the blood clot over 12-24 hours to dissolve it. The patient is hospitalized during the treatment. After the clot is dissolved, a patient may require additional treatments to open up any narrowed areas of the blood vessel.
Venous Disease
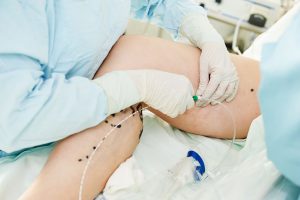 Endovenous Radiofrequency Ablation
Endovenous Radiofrequency Ablation
During radiofrequency ablation, a small catheter is thread into the malfunctioning vein through a tiny incision. The catheter then heats up the vein walls causing the vein to collapse and close. The blood is then rerouted to healthier properly functioning veins. The patient is able to return to most normal activities right away.
Sclerotherapy
Sclerotherapy is the injection of a chemical irritant through a tiny needle directly into smaller veins such as telangiectasia (spider veins) causing them to shrink and close.
DVT Thrombolysis
Catheter directed thrombolysis and thrombectomy have an increasing role in the treatment of Deep Vein Thrombosis (DVT). Depending on the severity, location, and acuity of clot, different approaches may be taken but generally a small catheter is passed into the vein and a clot busting drug is delivered into the clot (thrombolysis) potentially followed by passage of a device which mechanically breaks up and sucks out the clot (thrombectomy).
IVC Filter Placement
When there is concern that part of the clot in the leg, DVT, may break off and head to the lungs or heart, an inferior vena cava (IVC) filter can be placed. Usually these are placed temporarily. Using imaging guidance, the interventional radiologist places the IVC filter, which acts like a sieve, into the IVC, the largest vein in the abdomen, to catch any possible traveling clots.
Interventional Oncology
Chemoembolization
Transarterial chemoembolization (TACE) is used to treat certain types of inoperable primary liver cancer. Through a tiny hole in the groin or wrist, an interventionalist threads a catheter, thin tube, into the blood vessels supplying the liver tumor. The catheter delivers a high dose of a cancer-killing drug (chemotherapy) directly to the tumor. The chemotherapy is attached to small particles which then serve to block the artery, starving the tumor of its blood supply and preventing the chemotherapy from washing away and affecting normal healthy cells throughout the rest of the body.
Y-90 Embolization
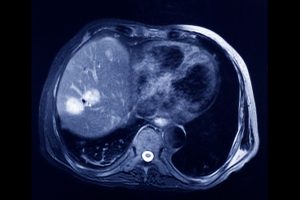 Radioembolization, also known as Selective Internal Radiation Therapy (SIRT) is very similar to chemoembolization but with injection of small spheres of radioactive substance. It is used to treat both primary and certain metastatic liver tumors. The radioactive isotope Yttrium-90, attached to tiny spheres, is delivered directly into a liver tumor through a small catheter thread through the blood vessels. The spheres become lodged in the tumor and emit high doses of radiation from within.
Radioembolization, also known as Selective Internal Radiation Therapy (SIRT) is very similar to chemoembolization but with injection of small spheres of radioactive substance. It is used to treat both primary and certain metastatic liver tumors. The radioactive isotope Yttrium-90, attached to tiny spheres, is delivered directly into a liver tumor through a small catheter thread through the blood vessels. The spheres become lodged in the tumor and emit high doses of radiation from within.
Microwave ablation
Microwave ablation is a minimally invasive technique that uses electromagnetic waves to generate heat to destroy tumors. Using CT or ultrasound guidance, a small needle electrode is advanced through a tiny skin incision directly into the tumor. Ablation is less traumatic than surgery, so it is an alternative for those patients or tumors which are not amenable to surgery. It is often performed on an outpatient basis.
Pain Management
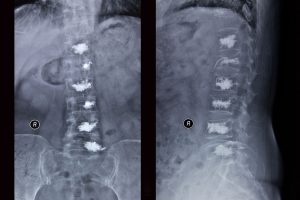 Kyphoplasty
Kyphoplasty
Kyphoplasty is a minimally invasive treatment for painful vertebral compression fractures that do not respond to conventional medical therapy. Using x-ray guidance, a small needle is inserted into the fractured vertebrae. A balloon is inserted through the needle and inflated to help restore height to the bone and create a cavity for subsequent cement injection. The procedure provides a near immediate relief in pain and can prevent further collapse of the vertebrae, helping to avoid the spine curvature sometimes seen with osteoporosis. A similar procedure is performed for sacral insufficiency fractures called sacroplasty.
Liver disease
Transjugular Intrahepatic Portosystemic Shunt (TIPS)
The blood vessels which drain the intestines, the portal veins, empty into the liver. When the liver hardens due to cirrhosis, blood flow is obstructed and pressure builds in the portal vein like a kinked hose leading to bleeding and/or ascites (excess fluid in the abdomen). A TIPS acts as a bypass around the hardened liver. An interventionalist enters a blood vessel at the neck through a small incision, using x-rays, a catheter is guided through the blood vessel, through the heart, and into the liver. From there a needle is passed through the liver into the portal vein. Using that access, the interventional connects the portal vein to the hepatic vein which eventually drains into the heart, bypassing the diseased liver. Patients are kept in the hospital for a few days afterwards to assess the success of the complex treatment and monitor for any complications.
Kidney failure
 Hemodialysis Access and AVF maintenance
Hemodialysis Access and AVF maintenance
When patients reach the final stage of Chronic Kidney Disease (CKD), End Stage Renal Disease (ESRD), they will require renal replacement therapy. We are able to provide temporary hemodialysis catheter placement as well as maintain already established access points. An arteriovenous fistula is a surgically created connection between an artery and vein which “arterializes” the vein and creates enough blood flow in your vein to allow your blood to be circulated and filtered by a dialysis machine. If your AVF malfunctions or clots, a patient may not be able to receive adequate dialysis. We work with our referring nephrologists, dialysis centers, and patients to provide optimal surveillance, maintenance, and when necessary declot of AVFs.
Women’s Health
Pelvic venogram and embolization
Pelvic venous congestion syndrome is chronic pelvic vein and heaviness caused by faulty pelvic veins where blood flows backward into the pelvis. An interventionalist advances a small catheter into a blood vessel in the groin via a tiny incision and manipulates the catheter into the pelvic veins. Contrast is injected into the veins to confirm the abnormal flow. Once confirmed, the interventionalist closes the vein through various methods, often using a small coil, to force the blood to flow out from the pelvis through other normal healthy veins.
Uterine Fibroid Embolization (UFE)
UFE is a procedure to treat benign growths in the uterine wall by starving them of their blood supply. A small catheter is advanced through a blood vessel in the groin or wrist down into the uterine artery in the pelvis. Once there, tiny particles are injected to block the artery and cut off the fibroids from their oxygen and nutrition causing them to shrink. The procedure usually requires an overnight admission for pain management. Patients are discharged with oral pain medications and can usually return to normal activities in a week. Nine out of 10 women report significant if not complete resolution of symptoms.
Men’s Health
Varicocele embolization
Through a tiny incision in the groin, a thin catheter is passed through the vein and directed toward the abnormally enlarged malfunctioning vein in the pelvis. Once there, the interventionalist delivers tiny coils into the blood vessel to obstruct them and force blood flow through normal healthy veins. Patients are discharged home the same day.
Prostatic Artery Embolization
While surgical options exist for the management of benign prostatic hyperplasia (BPH), more and more patients are opting for a new procedure, Prostatic Artery Embolization (PAE), due to decreased recovery time, decreased pain, and decreased risk of sexual side effects. Using x-ray guidance, a small catheter is advanced through an artery in the groin into the blood vessel that supplies the prostate. Once identified, the blood vessel is occluded. Without nutrients and oxygen, the prostate shrinks.
